Fighting cancer with interdisciplinary science
Angles of attack
By Marcia Locke
Seek more
Read more about the Johnson Cancer Research Center in the latest issue of Conquest magazine.
How do tumors develop despite the body’s defenses? Why can the body stop some tumors from forming but not others? What makes cancerous cells live longer than normal cells and wreak havoc on the body? And how can we fight these processes?
Kansas State University researchers are searching for answers to these questions and more through the interdisciplinary Johnson Cancer Research Center in the College of Arts and Sciences.
The center’s faculty members span 20 departments in five colleges. They work to better understand cancer and find ways to prevent it, detect it earlier and treat it more successfully, while also training the next generation of scientists.
Helping the body fight breast cancer
The body’s immune system helps fight infections and diseases, including cancers. But cancerous cells can escape or evade the immune attack and develop into tumors. Immunotherapy treatment can boost the immune system so that it can find and attack cancer cells.

Left: Anna Zolkiewska is developing immunotherapies to treat breast cancer. She has discovered that a protein important to some breast cancers can be disabled to slow tumor growth.
Anna Zolkiewska, professor of biochemistry and molecular biophysics in the College of Arts and Sciences, is developing and improving immunotherapies for breast cancer. She studies immune cells that infiltrate and help destroy breast cancer cells. Her research is supported by more than $1.65 million from the National Cancer Institute and more than $300,000 from the Johnson Cancer Research Center with support from the Flossie E. West Memorial Trust.
Immunotherapies are very effective against some types of cancer but are less successful against breast tumors. Triple-negative breast cancer, a particularly aggressive form of the disease, is especially hard to treat with any method. A new immunotherapy called immune checkpoint blockade offers hope, but it is effective for only a portion of patients. Zolkiewska is getting closer to finding out why.
She has discovered that a cell-surface protein called ADAM12 is important in triple-negative breast cancers. When she disabled the ADAM12 gene, tumor growth slowed down. Most importantly, tumors lacking ADAM12 contained more cancer-fighting immune cells, especially T cells and B cells.
Zolkiewska also showed that eliminating ADAM12 in breast cancer cells made tumors more responsive to immune checkpoint blockade therapy. This clue could improve immunotherapy efficacy for more patients, but there is evidence that the response may be temporary and followed by acquired resistance. Zolkiewska plans to investigate this effect further. She also is exploring if other proteins from the ADAM family may play a role in recruiting immune cells to breast tumors.
Seeking answers in the tumor’s environment
Some researchers are seeking clues from the tumor’s environment to improve cancer therapies. The Johnson Cancer Research Center has established the Cancer Research Collaboration of Excellence in Tumor Microenvironment Studies.

Right: Brad Behnke studies manipulation of tumor oxygenation to improve cancer therapies.
Brad Behnke, professor of kinesiology and associate dean of research and graduate studies for the College of Health and Human Sciences, is leading the multidisciplinary collaboration. The members’ synergistic investigations examine how environmental conditions within tumors affect their development, growth and aggressiveness.
“Many conventional cancer therapies fail due to factors related to the tumor’s microenvironment,” Behnke said. “We want to identify microenvironment changes that cause cancer growth and therapy resistance, and devise methods to combat them.”
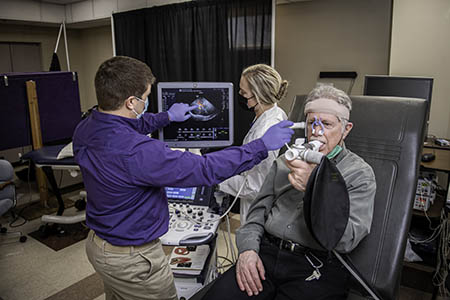
Left: Carl Ade, associate professor of kinesiology, researches cardiovascular damage caused by cancer treatments.
Other researchers involved are Amir Bahadori, associate professor in the Alan Levin Department of Mechanical and Nuclear Engineering in the Carl R. Ice College of Engineering; Carl Ade, associate professor of kinesiology in the College of Health and Human Sciences; David Poole, university distinguished professor of kinesiology in the College of Health and Human Sciences and of anatomy and physiology in the College of Veterinary Medicine; Chieko Azuma, clinical associate professor of radiation oncology in the College of Veterinary Medicine; and Wei-Wen Hsu, associate professor of statistics in the College of Arts and Sciences.
These esteemed experts have received individual research support from the National Institutes of Health, NASA, the American Cancer Society, the American Heart Association and additional organizations. Now they are teaming up to discover the changes that occur in the tumor microenvironment when it is exposed to different levels of radiation, oxygen pressures and vitamin D. They seek answers to four main questions.
- What DNA mutations occur in response to low-dose radiation? Low-level radiation exposure can cause DNA mutations that can develop into cancer. Exposure occurs in cancer patients undergoing radiation therapy as well as in radiation workers, astronauts and victims of radioactive material releases. The researchers are examining the biological mechanisms involved in such mutations and trying to develop therapeutics to stop them
- Does exercise increase oxygen in breast tumors and improve the response to radiation therapy? Tumors contain regions of hypoxic cells, which means they have low oxygen levels or pressures. This makes them resistant to radiation therapy. Aerobic exercise may increase a tumor’s blood circulation and oxygen levels and make it more susceptible to radiation therapy. This research will determine if aerobic exercise decreases breast tumor hypoxia and makes radiation therapy more effective.
- Does nitrate supplementation increase tumor oxygenation and decrease tumor growth? Another strategy to reduce tumor hypoxia might be to consume foods or supplements that elevate nitric oxide bioavailability. Beetroot juice is a concentrated source of nitrate and nitrite that is known to increase blood flow to some tissues. The researchers will determine if consuming beetroot juice raises tumor oxygen pressures, which could slow tumor growth and improve radiation therapy.
- How do ovarian tumors respond to different levels of vitamin D? Previous studies have shown that low levels of vitamin D in ovarian cancer patients are associated with larger tumors and lower survival rates. The scientists will determine if circulating vitamin D modifies the tumor microenvironment, and if so, how. The research could help predict ovarian cancer treatment complications, completion and overall survival
Attacking a killer virus
Human papillomavirus, or HPV, causes nearly all cervical cancers — more than half a million worldwide each year. But many people don’t know that most humans get HPV at some point in their lives and that it can cause cancers of both men’s and women’s genitals as well as the throat, skin and other body parts.

Right: Nicholas Wallace studies human papillomavirus which is a very common virus that causes nearly all cervical cancers as well as other cancers in men and women.
Nicholas Wallace, associate professor of biology in the College of Arts and Sciences, wants to reduce the suffering caused by HPV by learning more about its biology. He studies how HPV converts normal cells into factories that make more of the virus and how this leads to the cells’ uncontrolled and rapid growth — cancer.
“Typically, HPV infections, and the changes associated with them, are quickly cleared by our immune system,” Wallace said. “But if the virus escapes the immune system and the changes become permanent, a tumor will form. By learning how HPV proteins manipulate cells, we can determine which cancers were definitely caused by HPV infection and predict effective treatments.”
Recently, Wallace’s lab discovered changes in specific genes that cause commonly used chemotherapies to not work in some patients. The researchers are using a nearly $455,000 grant from the National Cancer Institute to test a new drug to treat these chemotherapy-resistant tumors.
Training the next generation
K-State excels at getting students involved in research. A major university goal is to develop highly skilled citizens who can advance the well-being of Kansas, the nation and the world. The Johnson Cancer Research Center helps achieve that goal by investing in student research training.
Through the center’s competitive Cancer Research Award program undergraduate students receive faculty-mentored research experiences and monetary awards. Graduate students receive support for their summertime research endeavors.
In 2021, 27 undergraduate students received Cancer Research Awards. Some of their research projects include:
- Studying lung cancer cell growth.
- Developing safer methods to deliver drugs in the body.
- Characterizing genetic mutations.
- Designing inhibitors to cancer-causing genes.
The awards support research outside traditional science fields as well. One student is studying the Navajo approach to cancer and another is examining the ethical dimensions of cancer treatment decisions.
The students become integral parts of research teams and some even publish their research. Such experience helps K-State students stand out when applying to graduate and medical schools, which many awardees do successfully.